Nobody warns you about perimenopause properly. You might get a vague mention from your GP that “things start changing in your forties,” but the reality — the fatigue, the brain fog, the digestive chaos, the sleep that just stops working — that bit tends to arrive unannounced.
And then comes the supplement question. You start searching for something, anything, that might help. The results are overwhelming. Dozens of menopause supplements, all promising relief, most with ingredient lists that raise more questions than they answer.
So let’s be honest about what the evidence actually supports, which perimenopause supplements are worth your money, and which ones are just riding the wave of desperate demand.
What Actually Happens During Perimenopause
Perimenopause is the transition phase before menopause — it can start anywhere from your mid-thirties to your late forties and last for several years. During this time, oestrogen and progesterone levels fluctuate unpredictably before eventually declining.
These hormonal shifts affect far more than your cycle. They ripple through virtually every system in your body:
Energy and mood — Oestrogen influences serotonin and dopamine production. When levels drop, fatigue, low mood, irritability, and anxiety often follow. Many women describe it as a tiredness that sleep doesn’t fix.
Sleep — Falling oestrogen disrupts your body’s temperature regulation and melatonin production. Night sweats and insomnia are two of the most reported perimenopause symptoms, and the knock-on effects of poor sleep compound everything else.
Brain function — Oestrogen supports cognitive function, memory, and concentration. The brain fog that many women experience during perimenopause is real, measurable, and incredibly frustrating.
Bone density — Oestrogen plays a protective role in bone health. As levels decline, bone loss accelerates. This is why osteoporosis risk increases significantly after menopause.
Gut health — Hormonal fluctuations directly affect gut motility and microbiome balance. Bloating, digestive discomfort, and changes in bowel habits are common during perimenopause but rarely discussed.
Skin and hair — Collagen production slows, skin becomes drier, and hair may thin. The connection between gut health and skin becomes particularly relevant during this time — when your digestion is disrupted, your skin often shows it.
Understanding these changes is important because it tells you what to look for in supplements. You’re not just managing hot flushes — you’re supporting a body going through a fundamental hormonal shift that affects energy, cognition, bones, digestion, and mood simultaneously.
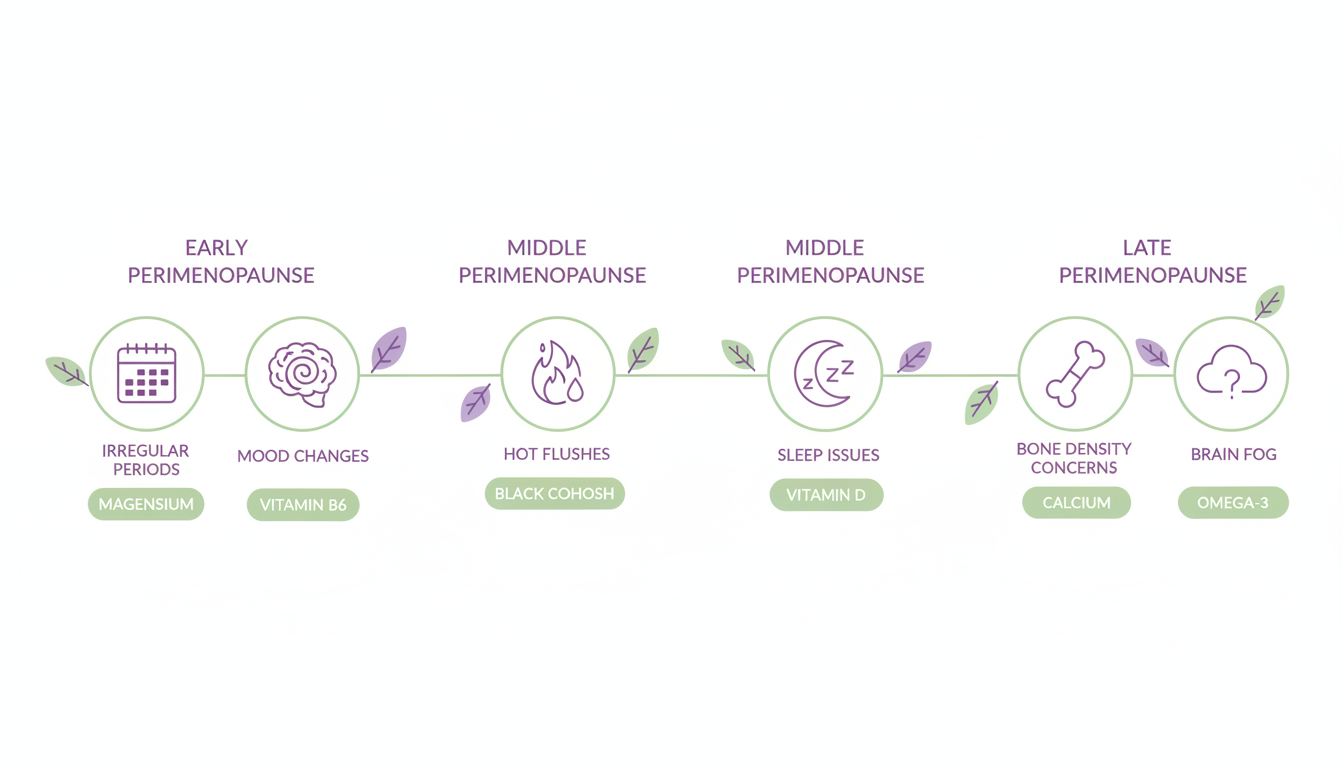
The Perimenopause Supplements That Actually Matter
Not every vitamin and mineral is equally relevant here. These are the ones with the strongest evidence base for the specific challenges perimenopause brings.
Magnesium
If there’s one mineral to prioritise during perimenopause, it’s this one. Magnesium supports over 300 biochemical reactions including sleep regulation, muscle relaxation, mood stability, and bone health — all of which take a hit during hormonal transition. Studies show that magnesium supplementation can improve sleep quality, reduce anxiety, and ease muscle cramps. Most women in the UK don’t get enough from diet alone, and the deficit becomes more significant during perimenopause when demand increases.
Magnesium supports over 300 biochemical reactions in the body — including sleep, mood, and bone health — yet most women in the UK don’t get enough from diet alone, and the deficit becomes more significant during perimenopause when demand increases.
Calcium — Bone density loss accelerates as oestrogen declines. Calcium is essential for slowing this process, but it works best alongside magnesium and weight-bearing exercise — calcium alone isn’t enough. Getting it through food and daily supplements (rather than mega-dose tablets) supports better absorption.
Vitamin B6
Plays a critical role in neurotransmitter production, including serotonin and GABA, both of which affect mood, anxiety, and sleep. B6 also supports your body’s production of melatonin, which is why it can help with the sleep disruption that perimenopause brings. Research has also shown that adequate B6 intake may help reduce the severity of PMS symptoms during the irregular cycles that characterise perimenopause.
Vitamin B12
Essential for energy production, nervous system function, and red blood cell formation. B12 deficiency causes fatigue that no amount of rest will fix — and absorption can decline with age, making supplementation increasingly important from your forties onwards. If you eat plant-based, supplementation is non-negotiable at any age, but especially during perimenopause.
Folate — Works in partnership with B12 to support cell production and neurological function. Low folate is linked to fatigue, mood changes, and cognitive difficulties — all symptoms that overlap with perimenopause, which is why deficiency often goes unrecognised during this phase.
Omega-3 DHA
The evidence for omega-3 during perimenopause is compelling. DHA supports brain function (directly addressing the fog and concentration issues), has anti-inflammatory properties that may reduce joint pain and stiffness, and supports cardiovascular health — which becomes a greater concern as oestrogen’s protective effects diminish. Some studies also suggest omega-3 may reduce the frequency and intensity of hot flushes, though the evidence there is still emerging.
Digestive enzymes and prebiotics
This one gets overlooked in almost every perimenopause supplement guide, and it shouldn’t. Hormonal changes directly disrupt gut function — slowing motility, altering the microbiome, and reducing digestive enzyme production. Supporting your gut during this transition isn’t optional — it’s what allows your body to actually absorb the other nutrients you’re taking. Prebiotic fibre feeds the beneficial bacteria that are struggling to maintain balance, and digestive enzymes ensure you’re breaking down food efficiently despite the hormonal headwinds.
What About HRT?
This article isn’t about whether to take HRT — that’s a conversation between you and your GP. But it’s worth saying that supplements and HRT aren’t mutually exclusive.
HRT addresses the root cause (declining hormones) directly. Nutritional supplementation addresses the downstream effects and supports the body systems that hormonal changes affect. Many women benefit from both.
Whether or not you’re on HRT, your body still needs adequate magnesium, B vitamins, calcium, omega-3, and digestive support. These aren’t replacements for hormone therapy — they’re foundations that support your health regardless of what else you’re doing.
Why a Protein Powder Can Do More Than You’d Expect
Here’s the practical argument. During perimenopause, your body needs more of several key nutrients at exactly the time when you’re least likely to have the energy or headspace to manage a complicated supplement routine.
Most women we speak to are already taking — or trying to remember to take — three to five separate supplements. Magnesium tablets, B-complex, omega-3 capsules, calcium, maybe a probiotic. That’s a lot of pills, a lot of expense, and realistically, a lot of forgotten doses.
A well-formulated protein powder can consolidate several of those into a single daily habit. Not all of them — but more than you might think.
Our vegan protein includes magnesium, calcium, B6, B12, folate, and omega-3 DHA alongside 20g of pea protein isolate. It also includes five digestive enzymes, live cultures, and prebiotic fibre from chicory root — directly supporting the gut disruption that perimenopause causes. Coconut MCT oil adds sustained energy without relying on caffeine or sugar.
That’s not a menopause supplement. It’s a daily protein shake that happens to cover several of the most critical nutritional gaps of perimenopause in a single scoop. The protein itself is important too — maintaining muscle mass becomes harder as oestrogen declines, and adequate protein intake is one of the most effective ways to slow that process.
Menopause Supplements to Be Wary Of
The menopause supplement market is booming, and not everything on the shelf deserves to be there.
Proprietary blends with undisclosed doses — If a product lists “menopause blend” without telling you how much of each ingredient is included, you can’t assess whether the doses are meaningful. Transparency matters, especially when you’re targeting specific deficiencies.
Mega-dose single-nutrient products — More isn’t always better. Very high doses of B6 can cause nerve damage over time. Excessive calcium without magnesium can cause problems. Sensible, balanced supplementation beats dramatic single-nutrient approaches.
Products relying entirely on phytoestrogens — Soy isoflavones, red clover, and black cohosh have some evidence for managing hot flushes, but the results are inconsistent and they don’t address the broader nutritional needs of perimenopause. They might help with one symptom while leaving everything else unsupported.
Anything making dramatic claims — “Reverse menopause symptoms,” “eliminate hot flushes naturally,” “turn back the clock.” Perimenopause is a natural biological process, not a disease to cure. Good supplements support your body through the transition — they don’t promise to stop it.
Supporting Yourself Beyond Supplements
Supplements work best as part of a broader approach. A few things that make a genuine difference during perimenopause:
Protein at every meal — Muscle mass declines with falling oestrogen. Adequate protein intake (1.2 to 1.6g per kilogram of body weight) helps maintain muscle, supports bone health, and improves satiety. A high protein breakfast is a particularly effective place to start — it stabilises blood sugar and sets a steadier energy tone for the rest of the day.
Weight-bearing exercise — Walking, resistance training, yoga, dancing — anything that puts load on your bones stimulates bone density maintenance. Combined with calcium and magnesium, it’s the most effective approach to long-term bone health.
Gut health attention — Your gut microbiome is directly affected by hormonal changes. Prebiotic fibre, fermented foods, and plant-based nutrition that’s gentle on your digestive system all help maintain the gut environment that allows everything else to work properly.
Sleep hygiene — Easier said than done when night sweats are involved, but the basics still help. Consistent schedule, cool bedroom, limited screens before bed, and magnesium in the evening.
The Bottom Line
Perimenopause supplements don’t need to be complicated. Focus on the nutrients with the strongest evidence — magnesium, B vitamins, calcium, omega-3, and digestive support — and find a practical way to get them consistently.
Whether that’s a thoughtful combination of individual supplements or a well-formulated daily protein shake that covers multiple bases at once, the goal is the same: give your body what it needs to navigate this transition without feeling like everything’s falling apart.
You’re not broken. Your body is changing. The least you can do is meet it halfway with proper nutrition.
References
- British Menopause Society. (2022). Prevention and treatment of osteoporosis in women. BMS Consensus Statement. View source
- Faubion, S. S., Crandall, C. J., Davis, L., Kling, J. M., Larson, J. H., Lawyer, L., Pinkerton, J. V., Prager, E. A., Reed, S. D., Sobel, T. H., Thomas, S., Winter, H. G., & Kapoor, E. (2023). The 2023 nonhormone therapy position statement of The Menopause Society. Menopause, 30(6), 573–590. View source
- Marangoni, F., Cetin, I., Verduci, E., Canzone, G., Giovannini, M., Sieri, S., Porrini, M., & Poli, A. (2016). Maternal diet and nutrient requirements in pregnancy and breastfeeding. Nutrients, 8(10), 629. View source
- Arab, A., Rafie, N., Amani, R., & Shirani, F. (2023). The role of magnesium in sleep health: a systematic review of available literature. Biological Trace Element Research, 201(1), 121–128. View source
- Kapoor, E., Collazo-Clavell, M. L., & Faubion, S. S. (2017). Weight gain in women at midlife: a concise review of the pathophysiology and strategies for management. Mayo Clinic Proceedings, 92(10), 1552–1558. View source
- Neves, J. C., Rosa, M. I., Felippe, F., Zanette, C., & Simon, C. S. (2018). Effect of omega-3 supplements on vasomotor symptoms in menopausal women: a systematic review and meta-analysis. Climacteric, 21(6), 536–542. View source
- Mikkola, T. S., Pukkala, E., Lyytinen, H., Ylikorkala, O., & Gissler, M. (2021). Increased risk of breast cancer in perimenopausal women. British Journal of Cancer. View source






